
-
What's the connection between gum disease and diabetes?
posted: Apr. 23, 2024.

-
Every Day is Earth Day
posted: Apr. 16, 2024.

-
Dental Insurance Benefits
posted: Apr. 09, 2024.

-
Snowball Effect
posted: Apr. 02, 2024.

-
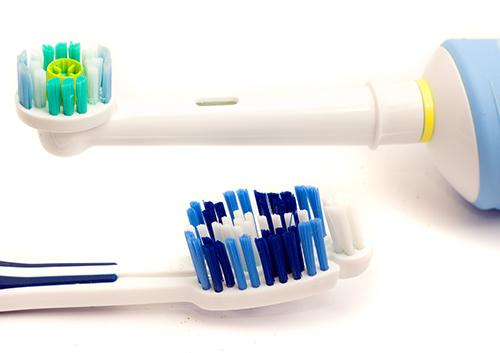
Electric or Manual Toothbrush: Why It Does (and Doesn't) Matter
posted: Mar. 26, 2024.
-
My teeth feel great. Do I still need to see the dentist?
posted: Mar. 19, 2024.

-
St. Patrick's Day: Celtic pride, green shamrocks, and lucky charms!
posted: Mar. 12, 2024.

-
Good Nutrition Leads to Healthy Mouths
posted: Mar. 05, 2024.

-
Tips for a Whiter Smile
posted: Feb. 27, 2024.

-
Should I use mouthwash?
posted: Feb. 20, 2024.

-
Choose Chocolate on Valentine's Day
posted: Feb. 13, 2024.

-
Sleep Apnea: What a Dentist Can Do
posted: Feb. 06, 2024.

-
Dental Fear in Children: Brought on by parents?
posted: Jan. 30, 2024.

-
Diabetes and Dental Care
posted: Jan. 23, 2024.

-
Famous Dentists in History
posted: Jan. 16, 2024.

-
Most Valuable Dental Treatments
posted: Jan. 09, 2024.

Our Location
Find us on the map
Thomasson Dental
1114 Gallatin Pk North, Madison, TN 37115
Phone: (615) 865-1732
Fax: (615) 606-7085
We are located in the greater Nashville area in the suburb of Madison, Tennessee. Our office is located at the red light at the intersection of One Mile Parkway and Gallatin Pk North, right next to Discount Motors.
Hours of Operation
Our Regular Schedule
Hours of Operation
Monday:
8:00 am-4:00 pm
Tuesday:
8:00 am-4:00 pm
Wednesday:
8:00 am-4:00 pm
Thursday:
8:00 am-4:00 pm
Friday:
8:00 AM - 12:00 PM (we are open every other Friday)
Saturday:
Closed
Sunday:
Closed
